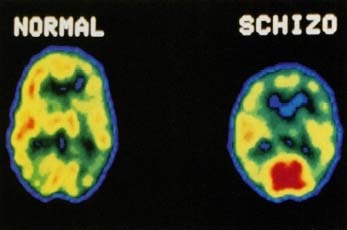
Schizophrenia
Schizophrenia (pronounced /ˌskɪtsɵˈfrɛniə/ or /ˌskɪtsɵˈfriːniə/) is a mental disorder
characterized by a disintegration of the process of thinking and of emotional responsiveness.[1 ]
It most commonly manifests as auditory hallucinations, paranoid or bizarre delusions, or
disorganized speech and thinking, and it is generally accompanied by significant social or
occupational dysfunction. Onset of symptoms typically occurs in young adulthood,[2] with a
global lifetime prevalence of around 1.5%.[3][4] Diagnosis is based on the patient's self-reported
experiences and observed behavior. No laboratory test for schizophrenia exists.[5 ]
Genetics, early environment, neurobiology, psychological and social processes appear to be
important contributory factors; some recreational and prescription drugs appear to cause or
worsen symptoms. Current psychiatric research is focused on the role of neurobiology, but this
inquiry has not isolated a single organic cause. As a result of the many possible combinations of
symptoms, there is debate about whether the diagnosis represents a single disorder or a
number of discrete syndromes. Despite the etymology of the term from the Greek roots
skhizein (σχίζειν, "to split") and phrēn, phren- (φρήν, φρεν-; "mind"), schizophrenia does not
imply a "split mind" and it is not the same as dissociative identity disorder—also known as
"multiple personality disorder" or "split personality"—a condition with which it is often confused
in public perception.[6]
Unusually high dopamine activity in the mesolimbic pathway of the brain has been found in
people with schizophrenia. The mainstay of treatment is antipsychotic medication; this type of
drug primarily works by suppressing dopamine activity. Dosages of antipsychotics are generally
lower than in the early decades of their use. Psychotherapy, and vocational and social
rehabilitation, are also important. In more serious cases—where there is risk to self and others
—involuntary hospitalization may be necessary, although hospital stays are shorter and less
frequent than they were in previous times.[7 ]
The disorder is thought mainly to affect cognition, but it also usually contributes to chronic
problems with behavior and emotion. People with schizophrenia are likely to have additional
(comorbid) conditions, including major depression and anxiety disorders;[8] the lifetime
occurrence of substance abuse is around 40%. Social problems, such as long-term
unemployment, poverty and homelessness, are common. Furthermore, the average life
expectancy of people with the disorder is 10 to 12 years less than those without, due to
increased physical health problems and a higher suicide rate (about 5%).[9][1 0]
Signs and symptoms
A person diagnosed with schizophrenia may experience hallucinations (most commonly hearing
voices), delusions (often bizarre or persecutory in nature), and disorganized thinking and
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 1/65
speech. The latter may range from loss of train of thought, to sentences only loosely connected
in meaning, to incoherence known as word salad in severe cases. There is often an observable
pattern of emotional difficulty, for example lack of responsiveness or motivation. Impairment in
social cognition is associated with schizophrenia, as are symptoms of paranoia, and social
isolation commonly occurs. In one uncommon subtype, the person may be largely mute, remain
motionless in bizarre postures, or exhibit purposeless agitation; these are signs of catatonia.
Late adolescence and early adulthood are peak years for the onset of schizophrenia. In 40% of
men and 23% of women diagnosed with schizophrenia, the condition arose before the age of
19.[1 1 ] These are critical periods in a young adult's social and vocational development. To
minimize the developmental disruption associated with schizophrenia, much work has recently
been done to identify and treat the prodromal (pre-onset) phase of the illness, which has been
detected up to 30 months before the onset of symptoms, but may be present longer.[1 2] Those
who go on to develop schizophrenia may experience the non-specific symptoms of social
withdrawal, irritability and dysphoria in the prodromal period,[1 3] and transient or self-limiting
psychotic symptoms in the prodromal phase before psychosis becomes apparent.[1 4]
Schneiderian classification
The psychiatrist Kurt Schneider (1887–1967) listed the forms of
psychotic symptoms that he thought distinguished schizophrenia
from other psychotic disorders. These are called first-rank
symptoms or Schneider's first-rank symptoms, and they include
delusions of being controlled by an external force; the belief that
thoughts are being inserted into or withdrawn from one's conscious
mind; the belief that one's thoughts are being broadcast to other
people; and hearing hallucinatory voices that comment on one's
thoughts or actions or that have a conversation with other
hallucinated voices.[1 5 ] Although they have significantly contributed
to the current diagnostic criteria, the specificity of first-rank
symptoms has been questioned. A review of the diagnostic studies
conducted between 1970 and 2005 found that these studies allow
neither a reconfirmation nor a rejection of Schneider's claims, and suggested that first-rank
symptoms be de-emphasized in future revisions of diagnostic systems.[1 6]
Positive and negative symptoms
Schizophrenia is often described in terms of positive and negative (or deficit) symptoms.[1 7 ]
The term positive symptoms refers to symptoms that most individuals do not normally
experience but are present in schizophrenia. They include delusions, auditory hallucinations,
and thought disorder, and are typically regarded as manifestations of psychosis. Negative
symptoms are things that are not present in schizophrenic persons but are normally found in
healthy persons, that is, symptoms that reflect the loss or absence of normal traits or abilities.
Common negative symptoms include flat or blunted affect and emotion, poverty of speech
(alogia), inability to experience pleasure (anhedonia), lack of desire to form relationships
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 2/65
(asociality), and lack of motivation (avolition). Research suggests that negative symptoms
contribute more to poor quality of life, functional disability, and the burden on others than do
positive symptoms.[1 8]
Diagnosis
Diagnosis is based on the self-reported experiences of the person, and abnormalities in behavior
reported by family members, friends or co-workers, followed by a clinical assessment by a
psychiatrist, social worker, clinical psychologist, mental health nurse or other mental health
professional. Psychiatric assessment includes a psychiatric history and some form of mental
status examination.[citation needed]
Standardized criteria
The most widely used standardized criteria for diagnosing schizophrenia come from the
American Psychiatric Association's Diagnostic and Statistical Manual of Mental Disorders,
version DSM-IV-TR, and the World Health Organization's International Statistical Classification
of Diseases and Related Health Problems, the ICD-10. The latter criteria are typically used in
European countries, while the DSM criteria are used in the United States and the rest of the
world, as well as prevailing in research studies. The ICD-10 criteria put more emphasis on
Schneiderian first-rank symptoms, although, in practice, agreement between the two systems is
high.[1 9]
According to the revised fourth edition of the Diagnostic and Statistical Manual of Mental
Disorders (DSM-IV-TR), to be diagnosed with schizophrenia, three diagnostic criteria must be
met:[5]
1. Characteristic symptoms: Two or more of the following, each present for much of the
time during a one-month period (or less, if symptoms remitted with treatment).
Delusions
Hallucinations
Disorganized speech, which is a manifestation of formal thought disorder
Grossly disorganized behavior (e.g. dressing inappropriately, crying frequently) or
catatonic behavior
Negative symptoms: Blunted affect (lack or decline in emotional response), alogia
(lack or decline in speech), or avolition (lack or decline in motivation)
If the delusions are judged to be bizarre, or hallucinations consist of hearing one
voice participating in a running commentary of the patient's actions or of hearing
two or more voices conversing with each other, only that symptom is required
above. The speech disorganization criterion is only met if it is severe enough to
substantially impair communication.
2. Social/occupational dysfunction: For a significant portion of the time since the
onset of the disturbance, one or more major areas of functioning such as work,
interpersonal relations, or self-care, are markedly below the level achieved prior to the
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 3/65
onset.
3. Duration: Continuous signs of the disturbance persist for at least six months. This sixmonth
period must include at least one month of symptoms (or less, if symptoms remitted
with treatment).
If signs of disturbance are present for more than a month but less than six months, the
diagnosis of schizophreniform disorder is applied.[5 ] Psychotic symptoms lasting less than a
month may be diagnosed as brief psychotic disorder, and various conditions may be classed as
psychotic disorder not otherwise specified. Schizophrenia cannot be diagnosed if symptoms of
mood disorder are substantially present (although schizoaffective disorder could be diagnosed),
or if symptoms of pervasive developmental disorder are present unless prominent delusions or
hallucinations are also present, or if the symptoms are the direct physiological result of a
general medical condition or a substance, such as abuse of a drug or medication.
Confu sion with other conditions
Psychotic symptoms may be present in several other mental disorders, including bipolar
disorder,[20] borderline personality disorder,[21 ] drug intoxication and drug-induced psychosis.
Delusions ("non-bizarre") are also present in delusional disorder, and social withdrawal in social
anxiety disorder, avoidant personality disorder and schizotypal personality disorder.
Schizophrenia is complicated with obsessive-compulsive disorder (OCD) considerably more
often than could be explained by pure chance, although it can be difficult to distinguish
compulsions that represent OCD from the delusions of schizophrenia.[22]
A more general medical and neurological examination may be needed to rule out medical
illnesses which may rarely produce psychotic schizophrenia-like symptoms,[5 ] such as
metabolic disturbance, systemic infection, syphilis, HIV infection, epilepsy, and brain lesions. It
may be necessary to rule out a delirium, which can be distinguished by visual hallucinations,
acute onset and fluctuating level of consciousness, and indicates an underlying medical illness.
Investigations are not generally repeated for relapse unless there is a specific medical indication
or possible adverse effects from antipsychotic medication.
"Schizophrenia" does not mean dissociative identity disorder—formerly and still widely known
as "multiple personalities"—despite the etymology of the word (Greek σχίζω = "I split").
Subtypes
The DSM-IV-TR contains five sub-classifications of schizophrenia, although the developers of
DSM-5 are recommending they be dropped from the new classification:[23]
Paranoid type: Where delusions and hallucinations are present but thought disorder,
disorganized behavior, and affective flattening are absent. (DSM code 295.3/ICD code
F20.0)
Disorganized type: Named hebephrenic schizophrenia in the ICD. Where thought
disorder and flat affect are present together. (DSM code 295.1/ICD code F20.1)
Catatonic type: The subject may be almost immobile or exhibit agitated, purposeless
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 4/65
movement. Symptoms can include catatonic stupor and waxy flexibility. (DSM code
295.2/ICD code F20.2)
Undifferentiated type: Psychotic symptoms are present but the criteria for paranoid,
disorganized, or catatonic types have not been met. (DSM code 295.9/ICD code F20.3)
Residual type: Where positive symptoms are present at a low intensity only. (DSM code
295.6/ICD code F20.5)
The ICD-10 defines two additional subtypes.
Post-schizophrenic depression: A depressive episode arising in the aftermath of a
schizophrenic illness where some low-level schizophrenic symptoms may still be present.
(ICD code F20.4)
Simple schizophrenia: Insidious and progressive development of prominent negative
symptoms with no history of psychotic episodes. (ICD code F20.6)
Controversies and research directions
The scientific validity of schizophrenia, and its defining symptoms such as delusions and
hallucinations, have been criticised.[24][25 ] In 2006, a group of consumers and mental health
professionals from the UK, under the banner of Campaign for Abolition of the Schizophrenia
Label, argued for a rejection of the diagnosis of schizophrenia based on its heterogeneity and
associated stigma, and called for the adoption of a biopsychosocial model. Other UK
psychiatrists opposed the move arguing that the term schizophrenia is a useful, even if
provisional concept.[26][27 ]
Similarly, there is an argument that the underlying issues would be better addressed as a
spectrum of conditions[28] or as individual dimensions along which everyone varies rather than
by a diagnostic category based on an arbitrary cut-off between normal and ill.[29] This approach
appears consistent with research on schizotypy, and with a relatively high prevalence of
psychotic experiences, mostly non-distressing delusional beliefs, among the general
public.[30][31 ][32] In concordance with this observation, psychologist Edgar Jones, and
psychiatrists Tony David and Nassir Ghaemi, surveying the existing literature on delusions,
pointed out that the consistency and completeness of the definition of delusion have been found
wanting by many; delusions are neither necessarily fixed, nor false, nor involve the presence of
incontrovertible evidence.[33][34][35 ]
Nancy Andreasen, a leading figure in schizophrenia research, has criticized the current DSM-IV
and ICD-10 criteria for sacrificing diagnostic validity for the sake of artificially improving
reliability. She argues that overemphasis on psychosis in the diagnostic criteria, while improving
diagnostic reliability, ignores more fundamental cognitive impairments that are harder to assess
due to large variations in presentation.[36][37 ] This view is supported by other
psychiatrists.[38] In the same vein, Ming Tsuang and colleagues argue that psychotic symptoms
may be a common end-state in a variety of disorders, including schizophrenia, rather than a
reflection of the specific etiology of schizophrenia, and warn that there is little basis for
regarding DSM’s operational definition as the "true" construct of schizophrenia.[28]
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 5/65
Neuropsychologist Michael Foster Green went further in suggesting the presence of specific
neurocognitive deficits may be used to construct phenotypes that are alternatives to those that
are purely symptom-based. These deficits take the form of a reduction or impairment in basic
psychological functions such as memory, attention, executive function and problem
solving.[39][40]
The exclusion of affective components from the criteria for schizophrenia, despite their ubiquity
in clinical settings, has also caused contention. This exclusion in the DSM has resulted in a
"rather convoluted" separate disorder—schizoaffective disorder.[38] Citing poor interrater
reliability, some psychiatrists have totally contested the concept of schizoaffective disorder as a
separate entity.[41 ][42] The categorical distinction between mood disorders and schizophrenia,
known as the Kraepelinian dichotomy, has also been challenged by data from genetic
epidemiology.[43]
An approach broadly known as the anti-psychiatry movement, most active in the 1960s,
opposes the orthodox medical view of schizophrenia as an illness.[44][page needed] Psychiatrist
Thomas Szasz argues that psychiatric patients are individuals with unconventional thoughts and
behavior that society diagnoses as a method of social control, and therefore the diagnosis of
"schizophrenia" is merely a form of social construction.[45] The Hearing Voices Movement
argues that many people diagnosed as psychotic need their experiences to be accepted and
valued rather than medicalized.
Causes
Main article: Causes of schizophrenia
While the reliability of the diagnosis introduces difficulties in
measuring the relative effect of genes and environment (for
example, symptoms overlap to some extent with severe
bipolar disorder or major depression), evidence suggests
that genetic and environmental factors can act in
combination to result in schizophrenia.[47 ] Evidence
suggests that the diagnosis of schizophrenia has a significant
heritable component but that onset is significantly influenced
by environmental factors or stressors.[48] The idea of an
inherent vulnerability (or diathesis) in some people, which
can be unmasked by biological, psychological or
environmental stressors, is known as the stress-diathesis
model.[49] An alternative idea that biological, psychological
and social factors are all important is known as the "biopsychosocial" model.
Genetic
Estimates of the heritability of schizophrenia tend to vary owing to the difficulty of separating
the effects of genetics and the environment although twin and adoption studies have suggested
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 6/65
a high level of heritability (the proportion of variation between individuals in a population that is
influenced by genetic factors).[5 0] It has been suggested that schizophrenia is a condition of
complex inheritance, with many different potential genes each of small effect, with different
pathways for different individuals. Some have suggested that several genetic and other risk
factors need to be present before a person becomes affected but this is still uncertain.[5 1 ]
Candidate genes linked to an increased risk of schizophrenia and bipolar disorder as found in
recent genome wide association studies appear to be partly separate and partly overlapping
between the two disorders[5 2] Metaanalyses of genetic linkage studies have produced evidence
of chromosomal regions increasing susceptibility,[5 3] which interacts directly with the Disrupted
in Schizophrenia 1 (DISC1) gene protein[5 4] more recently the zinc finger protein 804A.[5 5 ] has
been implicated as well as the chromosome 6 HLA region.[56] However, a large and
comprehensive genetic study found no evidence of any significant association with any of 14
previously identified candidate genes.[5 7 ] Schizophrenia, in a small minority of cases, has been
associated with rare deletions or duplications of tiny DNA sequences (known as copy number
variants) disproportionately occurring within genes involved in neuronal signaling and brain
development/human cognitive, behavioral, and psychological variation.[58][5 9][60] Relations
have been found between autism and schizophrenia based on duplications and deletions of
chromosomes; research showed that schizophrenia and autism are significantly more common
in combination with 1q21.1 deletion syndrome, velo-cardio-facial syndrome and Phelan-
McDermid syndrome. Duplications of parts of the chrmosomes which are opposites of these
syndromes show more autism-results. Research on autism/schizophrenia relations for
chromosome 15 (15q13.3), chromosome 16 (16p13.1) and chromosome 17 (17p12) are
inconclusive.[61 ]
Assuming a hereditary genetic basis, one question for evolutionary psychology is why genes
that increase the likelihood of the condition evolved, assuming the condition would have been
maladaptive from an evolutionary/reproductive point of view. One theory implicates genes
involved in the evolution of language and human nature, but so far all theories have been
disproved or remain unsubstantiated.[62][63]
Prenatal
Causal factors are thought to initially come together in early neurodevelopment to increase the
risk of later developing schizophrenia. One curious finding is that people diagnosed with
schizophrenia are more likely to have been born in winter or spring, (at least in the northern
hemisphere).[64] There is now evidence that prenatal exposure to infections increases the risk
for developing schizophrenia later in life, providing additional evidence for a link between in
utero developmental pathology and risk of developing the condition.[65 ]
Social
Living in an urban environment has been consistently found to be a risk factor for
schizophrenia.[66][67 ] Social disadvantage has been found to be a risk factor, including
poverty[68] and migration related to social adversity, racial discrimination, family dysfunction,
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 7/65
St r u ct u r e of a t y pi ca l ch em i ca l sy n a pse
Post sy n a pt ic
den sit y
V olt a g eg
a ted Ca ++
ch a n n el
Sy n a pt ic
v esicle
Reu pta ke
pu m p
Recept or
Neu r otr a n sm it t er
A x on t er m in a l
Sy n a pt ic cl eft
Den dr it e
unemployment or poor housing conditions.[69] Childhood experiences of abuse or trauma have
also been implicated as risk factors for a diagnosis of schizophrenia later in life.[7 0][7 1 ]
Parenting is not held responsible for schizophrenia but unsupportive dysfunctional relationships
may contribute to an increased risk.[7 2][7 3]
Substance Abu se
In a recent study of people with
schizophrenia and a substance
abuse disorder, over a ten year
period, "substantial proportions
were above cutoffs selected by
dual diagnosis clients as indicators
of recovery."[7 4] Although about
half of all patients with
schizophrenia use drugs or
alcohol, and the vast majority use
tobacco, a clear causal connection
between drug use and
schizophrenia has been difficult to
prove. The two most often used
explanations for this are
"substance use causes
schizophrenia" and "substance use
is a consequence of
schizophrenia", and they both
may be correct.[7 5 ] A 2007 metaanalysis
estimated that cannabis
use is statistically associated with
a dose-dependent increase in risk
of development of psychotic
disorders, including schizophrenia,
though the authors admit that some uncertainty about causality still remains.[7 6] For example,
cannabis use has increased dramatically in several countries over the past few decades, though
contrary to predictions the rates of psychosis and schizophrenia have generally not
increased.[7 7 ][7 8][7 9]
Psychotic individuals may also use drugs to cope with unpleasant states such as depression,
anxiety, boredom and loneliness, because drugs increase "feel-good" neurotransmitters
level.[80] Various studies have shown that amphetamines increases the concentrations of
dopamine in the synaptic cleft, thereby heightening the response of the post-synaptic
neuron.[81 ] However, regarding psychosis itself, it is well understood that methamphetamine
and cocaine use can result in methamphetamine- or cocaine-induced psychosis that present
very similar symptomatology (sometimes even misdiagnosed as schizophrenia) and may persist
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 8/65
even when users remain abstinent.[82] The same can also be said for alcohol-induced psychosis,
though to a somewhat lesser extent.[83][84][85 ]
Mechanisms
Psych ological
A number of psychological mechanisms have been implicated in the development and
maintenance of schizophrenia. Cognitive biases that have been identified in those with a
diagnosis or those at risk, especially when under stress or in confusing situations, include
excessive attention to potential threats, jumping to conclusions, making external attributions,
impaired reasoning about social situations and mental states, difficulty distinguishing inner
speech from speech from an external source, and difficulties with early visual processing and
maintaining concentration.[86][87 ][88][89] Some cognitive features may reflect global
neurocognitive deficits in memory, attention, problem-solving, executive function or social
cognition, while others may be related to particular issues and experiences.[7 2][90]
Despite a common appearance of "blunted affect", recent findings indicate that many individuals
diagnosed with schizophrenia are emotionally responsive, particularly to stressful or negative
stimuli, and that such sensitivity may cause vulnerability to symptoms or to the
disorder.[91 ][91 ][92][93] Some evidence suggests that the content of delusional beliefs and
psychotic experiences can reflect emotional causes of the disorder, and that how a person
interprets such experiences can influence symptomatology.[94][95 ][96][97 ] The use of "safety
behaviors" to avoid imagined threats may contribute to the chronicity of delusions.[98] Further
evidence for the role of psychological mechanisms comes from the effects of psychotherapies on
symptoms of schizophrenia.[99]
Neural
Studies using neuropsychological tests and brain imaging technologies such as fMRI and PET to
examine functional differences in brain activity have shown that differences seem to most
commonly occur in the frontal lobes, hippocampus and temporal lobes.[1 00] These differences
have been linked to the neurocognitive deficits often associated with schizophrenia.[1 01 ]
Particular focus has been placed upon the function of
dopamine in the mesolimbic pathway of the brain. This focus
largely resulted from the accidental finding that a drug group
which blocks dopamine function, known as the
phenothiazines, could reduce psychotic symptoms. It is also
supported by the fact that amphetamines, which trigger the
release of dopamine, may exacerbate the psychotic
symptoms in schizophrenia.[1 02] An influential theory,
known as the Dopamine hypothesis of schizophrenia,
proposed that excess activation of D2 receptors was the
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 9/65
cause of (the positive symptoms of) schizophrenia. Although postulated for about 20 years
based on the D2 blockade effect common to all antipsychotics, it was not until the mid-1990s
that PET and SPET imaging studies provided supporting evidence. This explanation is now
thought to be simplistic, partly because newer antipsychotic medication (called atypical
antipsychotic medication) can be equally effective as older medication (called typical
antipsychotic medication), but also affects serotonin function and may have slightly less of a
dopamine blocking effect.[1 03]
Interest has also focused on the neurotransmitter glutamate and the reduced function of the
NMDA glutamate receptor in schizophrenia. This has largely been suggested by abnormally low
levels of glutamate receptors found in postmortem brains of people previously diagnosed with
schizophrenia[1 04] and the discovery that the glutamate blocking drugs such as phencyclidine
and ketamine can mimic the symptoms and cognitive problems associated with the
condition.[1 05] The fact that reduced glutamate function is linked to poor performance on tests
requiring frontal lobe and hippocampal function and that glutamate can affect dopamine
function, all of which have been implicated in schizophrenia, have suggested an important
mediating (and possibly causal) role of glutamate pathways in schizophrenia.[1 06] Positive
symptoms fail however to respond to glutamatergic medication.[1 07 ]
There have also been findings of differences in the size and structure of certain brain areas in
schizophrenia. A 2006 metaanlaysis of MRI studies found that whole brain and hippocampal
volume are reduced and that ventricular volume is increased in patients with a first psychotic
episode relative to healthy controls. The average volumetric changes in these studies are
however close to the limit of detection by MRI methods, so it remains to be determined
whether schizophrenia is a neurodegenerative process that begins at about the time of
symptom onset, or whether it is better characterised as a neurodevelopmental process that
produces abnormal brain volumes at an early age.[1 08] In first episode psychosis typical
antipsychotics like haloperidol were associated with significant reductions in gray matter
volume, whereas atypical antipsychotics like olanzapine were not.[1 09] Studies in non-human
primates found gray and white matter reductions for both typical and atypical
antipsychotics.[1 1 0]
A 2009 meta-analysis of diffusion tensor imaging studies identified two consistent locations of
reduced fractional anisotropy (roughly the level of organization of neural connections) in
schizophrenia. The authors suggest that two networks of white matter tracts may be affected in
schizophrenia, with the potential for "disconnection" of the gray matter regions which they
link.[1 1 1 ] During fMRI studies, greater connectivity in the brain's default network and taskpositive
network has been observed in patients diagnosed with schizophrenia, and may reflect
excessive attentional orientation toward introspection and toward extrospection, respectively.
The greater anti-correlation between the two networks suggests excessive rivalry between the
networks.[1 1 2]
Screening and prevention
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 10/65
There are no reliable markers for the later development of schizophrenia although research is
being conducted into how well a combination of genetic risk plus non-disabling psychosis-like
experience predicts later diagnosis.[1 1 3] People who fulfill the 'ultra high-risk mental state'
criteria, that include a family history of schizophrenia plus the presence of transient or selflimiting
psychotic experiences, have a 20–40% chance of being diagnosed with the condition
after one year.[1 1 4] The use of psychological treatments and medication has been found
effective in reducing the chances of people who fulfill the 'high-risk' criteria from developing fullblown
schizophrenia.[1 1 5 ] However, the treatment of people who may never develop
schizophrenia is controversial,[1 1 6] in light of the side-effects of antipsychotic medication;
particularly with respect to the potentially disfiguring tardive dyskinesia and the rare but
potentially lethal neuroleptic malignant syndrome.[1 1 7 ] The most widely used form of
preventative health care for schizophrenia takes the form of public education campaigns that
provide information on risk factors and early symptoms, with the aim to improve detection and
provide treatment earlier for those experiencing delays.[1 1 8] The new clinical approach early
intervention in psychosis is a secondary prevention strategy to prevent further episodes and
prevent the long term disability associated with schizophrenia.
Management
Main article: Treatment of schizophrenia
The effectiveness of schizophrenia treatment is often
assessed using standardized methods, one of the most
common being the Positive and Negative Syndrome Scale
(PANSS).[1 1 9] Management of symptoms and improving
function is thought to be more achievable than a cure.
Treatment was revolutionized in the mid-1950s with the
development and introduction of chlorpromazine.[1 20] A
recovery model is increasingly adopted, emphasizing hope,
empowerment and social inclusion.[1 21 ]
Hospitalization may occur with severe episodes of
schizophrenia. This can be voluntary or (if mental health
legislation allows it) involuntary (called civil or involuntary commitment). Long-term inpatient
stays are now less common due to deinstitutionalization, although can still occur.[7 ] Following
(or in lieu of) a hospital admission, support services available can include drop-in centers, visits
from members of a community mental health team or Assertive Community Treatment team,
supported employment[1 22] and patient-led support groups.
In many non-Western societies, schizophrenia may only be treated with more informal,
community-led methods. Multiple international surveys by the World Health Organization over
several decades have indicated that the outcome for people diagnosed with schizophrenia in
non-Western countries is on average better there than for people in the West.[1 23]
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 11/65
Medication
The first line psychiatric treatment for schizophrenia is antipsychotic medication.[1 24] These
can reduce the positive symptoms of psychosis. Most antipsychotics take around 7–14 days to
have their main effect. Currently available antipsychotics fail, however, to significantly
ameliorate the negative symptoms, and the improvements on cognition may be attributed to
the practice effect.[1 25 ][1 26][1 27 ][1 28]
The newer atypical antipsychotic drugs are usually preferred
for initial treatment over the older typical antipsychotic,
although they are expensive and are more likely to induce
weight gain and obesity-related diseases.[1 29] In 2005–
2006, results from a major randomized trial sponsored by
the US National Institute of Mental Health (Clinical
Antipsychotic Trials of Intervention Effectiveness, or
CATIE)[1 30] found that a representative first-generation
antipsychotic, perphenazine, was as effective as and more
cost-effective than several newer drugs taken for up to 18
months. The atypical antipsychotic which patients were
willing to continue for the longest, olanzapine, was associated
with considerable weight gain and risk of metabolic
syndrome. Clozapine was most effective for people with a
poor response to other drugs, but it had troublesome side
effects. Because the trial excluded patients with tardive dyskinesia, its relevance to these people
is unclear.[1 31 ]
Because of their reportedly lower risk of side effects that affect mobility, atypical antipsychotics
have been first-line treatment for early-onset schizophrenia for many years before certain
drugs in this class were approved by the Food and Drug Administration for use in children and
teenagers with schizophrenia. This advantage comes at the cost of an increased risk of metabolic
syndrome and obesity, which is of concern in the context of long-term use begun at an early
age. Especially in the case of children and teenagers who have schizophrenia, medication should
be used in combination with individual therapy and family-based interventions.[1 1 ]
Recent reviews have refuted the claim that atypical antipsychotics have fewer extrapyramidal
side effects than typical antipsychotics, especially when the latter are used in low doses or when
low potency antipsychotics are chosen.[1 32] Prolactin elevations have been reported in women
with schizophrenia taking atypical antipsychotics.[1 33] It remains unclear whether the newer
antipsychotics reduce the chances of developing neuroleptic malignant syndrome, a rare but
serious and potentially fatal neurological disorder most often caused by an adverse reaction to
neuroleptic or antipsychotic drugs.[1 34]
Response of symptoms to medication is variable: treatment-resistant schizophrenia is a term
used for the failure of symptoms to respond satisfactorily to at least two different
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 12/65
antipsychotics.[1 35 ] Patients in this category may be prescribed clozapine,[1 36] a medication of
superior effectiveness but several potentially lethal side effects including agranulocytosis and
myocarditis.[1 37 ] For other patients who are unwilling or unable to take medication regularly,
long-acting depot preparations of antipsychotics may be given every two weeks to achieve
control. The United States and Australia are two countries with laws allowing the forced
administration of this type of medication on those who refuse, but are otherwise stable and
living in the community.
Psych ological and social interventions
Psychotherapy is also widely recommended and used in the treatment of schizophrenia,
although services may often be confined to pharmacotherapy because of reimbursement
problems or lack of training.[1 38]
Cognitive behavioral therapy (CBT) is used to target specific symptoms[1 39][1 40][1 41 ] and
improve related issues such as self-esteem, social functioning, and insight. Although the results
of early trials were inconclusive[1 42] as the therapy advanced from its initial applications in the
mid 1990s, CBT has become an effective treatment to reduce positive and negative symptoms
of schizophrenia, as well as improving functioning.[1 43][1 44] However, in a 2010 article in
Psychological Medicine entitled, "Cognitive behavioral therapy for the major psychiatric
disorder: does it really work?",[1 45] Lynch, Laws & McKenna found that no trial employing both
blinding and psychological placebo has found CBT to be effective in either reducing symptoms or
preventing relapse in schizophrenia.
Another approach is cognitive remediation, a technique aimed at remediating the
neurocognitive deficits sometimes present in schizophrenia. Based on techniques of
neuropsychological rehabilitation, early evidence has shown it to be cognitively effective, with
some improvements related to measurable changes in brain activation as measured by
fMRI.[1 46][1 47 ] A similar approach known as cognitive enhancement therapy, which focuses on
social cognition as well as neurocognition, has shown efficacy.[1 48]
Family therapy or education, which addresses the whole family system of an individual with a
diagnosis of schizophrenia, has been consistently found to be beneficial, at least if the duration of
intervention is longer-term.[1 49][1 50][1 5 1 ] Aside from therapy, the effect of schizophrenia on
families and the burden on carers has been recognized, with the increasing availability of selfhelp
books on the subject.[1 5 2][1 5 3] There is also some evidence for benefits from social skills
training, although there have also been significant negative findings.[1 5 4][1 5 5] Some studies
have explored the possible benefits of music therapy and other creative
therapies.[1 5 6][1 5 7 ][1 58]
The Soteria model is alternative to inpatient hospital treatment using a minimal medication
approach. It is described as a milieu-therapeutic recovery method, characterized by its founder
as "the 24 hour a day application of interpersonal phenomenologic interventions by a
nonprofessional staff, usually without neuroleptic drug treatment, in the context of a small,
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 13/65
homelike, quiet, supportive, protective, and tolerant social environment."[1 59] Although
research evidence is limited, a 2008 systematic review found the programme equally as
effective as treatment with medication in people diagnosed with first and second episode
schizophrenia.[1 60]
Other
Electroconvulsive therapy is not considered a first line treatment but may be prescribed in
cases where other treatments have failed. It is more effective where symptoms of catatonia are
present,[1 61 ] and is recommended for use under NICE guidelines in the UK for catatonia if
previously effective, though there is no recommendation for use for schizophrenia
otherwise.[1 62] Psychosurgery has now become a rare procedure and is not a recommended
treatment.[1 63]
Service-user led movements have become integral to the recovery process in Europe and the
United States; groups such as the Hearing Voices Network and the Paranoia Network have
developed a self-help approach that aims to provide support and assistance outside the
traditional medical model adopted by mainstream psychiatry. By avoiding framing personal
experience in terms of criteria for mental illness or mental health, they aim to destigmatize the
experience and encourage individual responsibility and a positive self-image. Partnerships
between hospitals and consumer-run groups are becoming more common, with services
working toward remediating social withdrawal, building social skills and reducing
rehospitalization.[1 64]
Regular exercise can have healthful effects on both the physical and mental health and wellbeing
of individuals with schizophrenia.[1 65]
Prognosis
Course
Coordinated by the World Health Organization and published
in 2001, The International Study of Schizophrenia (ISoS) was
a long-term follow-up study of 1633 individuals diagnosed
with schizophrenia around the world. Of the 75% who were
available for follow-up, half had a favourable outcome, and
16% had a delayed recovery after an early unremitting
course. More usually, the course in the first two years
predicted the long-term course. Early social intervention was
also related to a better outcome. The findings were held as
important in moving patients, carers and clinicians away
from the prevalent belief of the chronic nature of the
condition.[1 66] A review of major longitudinal studies in
North America noted this variation in outcomes, although
outcome was on average worse than for other psychotic and
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 14/65
psychiatric disorders. A moderate number of patients with
schizophrenia were seen to remit and remain well; the review
raised the question that some may not require maintenance medication.[1 67 ]
A clinical study using strict recovery criteria (concurrent remission of positive and negative
symptoms and adequate social and vocational functioning continuously for two years) found a
recovery rate of 14% within the first five years.[1 68] A 5-year community study found that 62%
showed overall improvement on a composite measure of clinical and functional outcomes.[1 69]
World Health Organization studies have noted that individuals diagnosed with schizophrenia
have much better long-term outcomes in developing countries (India, Colombia and Nigeria)
than in developed countries (United States, United Kingdom, Ireland, Denmark, Czech
Republic, Slovakia, Japan, and Russia),[1 7 0] despite antipsychotic drugs not being widely
available.
Defining recovery
Rates are not always comparable across studies because exact definitions of remission and
recovery have not been widely established. A "Remission in Schizophrenia Working Group" has
proposed standardized remission criteria involving "improvements in core signs and symptoms
to the extent that any remaining symptoms are of such low intensity that they no longer
interfere significantly with behavior and are below the threshold typically utilized in justifying
an initial diagnosis of schizophrenia".[1 7 1 ] Standardized recovery criteria have also been
proposed by a number of different researchers, with the stated DSM definitions of a "complete
return to premorbid levels of functioning” or "complete return to full functioning" seen as
inadequate, impossible to measure, incompatible with the variability in how society defines
normal psychosocial functioning, and contributing to self-fulfilling pessimism and stigma.[1 7 2]
Some mental health professionals may have quite different basic perceptions and concepts of
recovery than individuals with the diagnosis, including those in the Consumer/Survivor/Ex-
Patient Movement.[1 7 3] One notable limitation of nearly all the research criteria is failure to
address the person's own evaluations and feelings about their life. Schizophrenia and recovery
often involve a continuing loss of self-esteem, alienation from friends and family, interruption of
school and career, and social stigma, "experiences that cannot just be reversed or
forgotten".[1 21 ] An increasingly influential model defines recovery as a process, similar to being
"in recovery" from drug and alcohol problems, and emphasizes a personal journey involving
factors such as hope, choice, empowerment, social inclusion and achievement.[1 21 ]
Predictors
Several factors have been associated with a better overall prognosis: Being female, rapid (vs.
insidious) onset of symptoms, older age of first episode, predominantly positive (rather than
negative) symptoms, presence of mood symptoms, and good pre-illness functioning.[1 7 4][1 7 5]
The strengths and internal resources of the individual concerned, such as determination or
psychological resilience, have also been associated with better prognosis.[1 67 ] The attitude and
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 15/65
level of support from people in the individual's life can have a significant impact; research
framed in terms of the negative aspects of this—the level of critical comments, hostility, and
intrusive or controlling attitudes, termed high 'Expressed emotion'—has consistently indicated
links to relapse.[1 7 6] Most research on predictive factors is correlational in nature, however,
and a clear cause-and-effect relationship is often difficult to establish.
Mortality
In a study of over 168,000 Swedish citizens undergoing psychiatric treatment, schizophrenia
was associated with an average life expectancy of approximately 80–85% of that of the general
population; women were found to have a slightly better life expectancy than men, and a
diagnosis of schizophrenia was associated with an overall better life expectancy than substance
abuse, personality disorder, heart attack and stroke.[1 7 7 ] Other identified factors include
smoking,[1 7 8] poor diet, little exercise and the negative health effects of psychiatric drugs.[9]
There is a higher than average suicide rate associated with schizophrenia. This has been cited at
10%, but a more recent analysis of studies and statistics revises the estimate at 4.9%, most
often occurring in the period following onset or first hospital admission.[1 7 9] Several times more
attempt suicide.[1 80] There are a variety of reasons and risk factors.[1 81 ][1 82]
Violence
The relationship between violent acts and schizophrenia is a contentious topic. Current research
indicates that the percentage of people with schizophrenia who commit violent acts is higher
than the percentage of people without any disorder, but lower than is found for disorders such
as alcoholism, and the difference is reduced or not found in same-neighbourhood comparisons
when related factors are taken into account, notably sociodemographic variables and substance
misuse.[1 83] Studies have indicated that 5% to 10% of those charged with murder in Western
countries have a schizophrenia spectrum disorder.[1 84][1 85 ][1 86]
The occurrence of psychosis in schizophrenia has sometimes been linked to a higher risk of
violent acts. Findings on the specific role of delusions or hallucinations have been inconsistent,
but have focused on delusional jealousy, perception of threat and command hallucinations. It
has been proposed that a certain type of individual with schizophrenia may be most likely to
offend, characterized by a history of educational difficulties, low IQ, conduct disorder, earlyonset
substance misuse and offending prior to diagnosis.[1 84]
Individuals with a diagnosis of schizophrenia are often the victims of violent crime—at least 14
times more often than they are perpetrators.[1 87 ][1 88] Another consistent finding is a link to
substance misuse, particularly alcohol,[1 89] among the minority who commit violent acts.
Violence by or against individuals with schizophrenia typically occurs in the context of complex
social interactions within a family setting,[1 90] and is also an issue in clinical services[1 91 ] and in
the wider community.[1 92]
Epidemiology
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 16/65
Schizophrenia occurs equally in males and
females, although typically appears earlier
in men—the peak ages of onset are 20–28
years for males and 26–32 years for
females.[2] Onset in childhood is much
rarer,[1 93] as is onset in middle- or old
age.[1 94] The lifetime prevalence of
schizophrenia—the proportion of
individuals expected to experience the
disease at any time in their lives—is commonly given at 1%. However, a 2002 systematic
review of many studies found a lifetime prevalence of 0.55%.[4] Despite the received wisdom
that schizophrenia occurs at similar rates worldwide, its prevalence varies across the world,[1 95]
within countries,[1 96] and at the local and neighbourhood level.[1 97 ] One particularly stable and
replicable finding has been the association between living in an urban environment and
schizophrenia diagnosis, even after factors such as drug use, ethnic group and size of social
group have been controlled for.[66] Schizophrenia is known to be a major cause of disability. In a
1999 study of 14 countries, active psychosis was ranked the third-most-disabling condition
after quadriplegia and dementia and ahead of paraplegia and blindness.[1 98]
History
Main article: History of schizophrenia
Accounts of a schizophrenia-like syndrome are thought to be rare in the historical record before
the 1800s, although reports of irrational, unintelligible, or uncontrolled behavior were common.
A detailed case report in 1797 concerning James Tilly Matthews, and accounts by Phillipe Pinel
published in 1809, are often regarded as the earliest cases of the illness in the medical and
psychiatric literature.[1 99] Schizophrenia was first described as a distinct syndrome affecting
teenagers and young adults by Bénédict Morel in 1853, termed démence précoce (literally
'early dementia'). The term dementia praecox was used in 1891 by Arnold Pick to in a case
report of a psychotic disorder. In 1893 Emil Kraepelin introduced a broad new distinction in the
classification of mental disorders between dementia praecox and mood disorder (termed manic
depression and including both unipolar and bipolar depression). Kraepelin believed that
dementia praecox was primarily a disease of the brain,[200] and particularly a form of
dementia, distinguished from other forms of dementia, such as Alzheimer's disease, which
typically occur later in life.[201 ]
The word schizophrenia—which translates roughly as "splitting of the mind" and comes from
the Greek roots schizein (σχίζειν, "to split") and phrēn, phren- (φρήν, φρεν-, "mind")[202]—
was coined by Eugen Bleuler in 1908 and was intended to describe the separation of function
between personality, thinking, memory, and perception. Bleuler described the main symptoms
as 4 A's: flattened Affect, Autism, impaired Association of ideas and Ambivalence.[203] Bleuler
realized that the illness was not a dementia as some of his patients improved rather than
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 17/65
deteriorated and hence proposed the term schizophrenia instead.
In the early 1970s, the diagnostic criteria for schizophrenia was the subject of a number of
controversies which eventually led to the operational criteria used today. It became clear after
the 1971 US-UK Diagnostic Study that schizophrenia was diagnosed to a far greater extent in
America than in Europe.[204] This was partly due to looser diagnostic criteria in the US, which
used the DSM-II manual, contrasting with Europe and its ICD-9. David Rosenhan's 1972 study,
published in the journal Science under the title On being sane in insane places, concluded that
the diagnosis of schizophrenia in the US was often subjective and unreliable.[205] These were
some of the factors in leading to the revision not only of the diagnosis of schizophrenia, but the
revision of the whole DSM manual, resulting in the publication of the DSM-III in
1980.{subscription required}[206]
The term schizophrenia is commonly misunderstood to mean that affected persons have a
"split personality". Although some people diagnosed with schizophrenia may hear voices and
may experience the voices as distinct personalities, schizophrenia does not involve a person
changing among distinct multiple personalities. The confusion arises in part due to the literal
interpretation of Bleuler's term schizophrenia. The first known misuse of the term to mean
"split personality" was in an article by the poet T. S. Eliot in 1933.[207 ]
Society and culture
Stigma
Social stigma has been identified as a major obstacle in the recovery of patients with
schizophrenia.[208] In a large, representative sample from a 1999 study, 12.8% of Americans
believed that individuals with schizophrenia were "very likely" to do something violent against
others, and 48.1% said that they were "somewhat likely" to. Over 74% said that people with
schizophrenia were either "not very able" or "not able at all" to make decisions concerning their
treatment, and 70.2% said the same of money management decisions.[209] The perception of
individuals with psychosis as violent has more than doubled in prevalence since the 1950s,
according to one meta-analysis.[21 0]
In 2002, the Japanese Society of Psychiatry and Neurology changed the term for schizophrenia
from Seishin-Bunretsu-Byo 精神分裂病 (mind-split-disease) to Tōgō-shitchō-shō 統合失調
症 (integration disorder) to reduce stigma,[21 1 ] The new name was inspired by the
biopsychosocial model, and it increased the percentage of cases in which patients were informed
of the diagnosis from 36.7% to 69.7% over three years.[21 2]
Iconic cu ltural depictions
The book and film A Beautiful Mind chronicled the life of John Forbes Nash, a Nobel Prizewinning
mathematician who was diagnosed with schizophrenia. The Marathi film Devrai
(featuring Atul Kulkarni) is a presentation of a patient with schizophrenia. The film, set in
Western India, shows the behavior, mentality, and struggle of the patient as well as his loved-
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 18/65
ones. Other factual books have been written by relatives on family members; Australian
journalist Anne Deveson told the story of her son's battle with schizophrenia in Tell Me I'm
Here,[21 3] later made into a movie. The book The Eden Express by Mark Vonnegut recounts his
struggle with schizophrenia and his recovering journey.
See also
Persecutory delusions
Catastrophic schizophrenia
References
1. "Schizophrenia" Concise Medical Dictionary. Oxford University Press, 2010. Oxford
Reference Online. Maastricht University Library. 29 June 2010 prepaid subscription only
2. ^ a b Castle D, Wessely S, Der G, Murray RM. The incidence of operationally defined
schizophrenia in Camberwell, 1965-84. The British Journal of Psychiatry. 1991;159:790–
4. doi:10.1192/bjp.159.6.790
. PMID 1790446
.
3. Bhugra D. The global prevalence of schizophrenia
. PLoS Medicine. 2005;2(5):e151; quiz e175. doi:10.1371/journal.pmed.0020151
. PMID 15916460
.
4. ^ a b Goldner EM, Hsu L, Waraich P, Somers JM. Prevalence and incidence studies of
schizophrenic disorders: a systematic review of the literature. Canadian Journal of
Psychiatry. 2002;47(9):833–43. PMID 12500753
.
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 19/65
5. ^ a b c d American Psychiatric Association (2000). "Schizophrenia"
. Diagnostic and statistical manual of mental disorders: DSM-IV. Washington, DC:
American Psychiatric Publishing, Inc.. ISBN 0-89042-024-6. Retrieved 2008-07-04.
6. Rathus, Spencer and Jeffrey Nevid. Abnormal Psychology. Prentice Hall; 1991. ISBN
0130052167. p. 228.
7. ^ a b Becker T, Kilian R. Psychiatric services for people with severe mental illness across
western Europe: what can be generalized from current knowledge about differences in
provision, costs and outcomes of mental health care?. Acta Psychiatrica Scandinavica
Supplement. 2006;429(429):9–16. doi:10.1111/j.1600-0447.2005.00711.x
. PMID 16445476
.
8. Sim K, Chua TH, Chan YH, Mahendran R, Chong SA. Psychiatric comorbidity in first
episode schizophrenia: a 2 year, longitudinal outcome study. Journal of Psychiatric
Research. 2006;40(7):656–63. doi:10.1016/j.jpsychires.2006.06.008
. PMID 16904688
.
9. ^ a b Brown S, Barraclough B, Inskip H. Causes of the excess mortality of schizophrenia.
British Journal of Psychiatry. 2000;177:212–7. doi:10.1192/bjp.177.3.212
. PMID 11040880
.
10. Palmer BA, Pankratz VS, Bostwick JM. The lifetime risk of suicide in schizophrenia: a
reexamination. Archives of General Psychiatry. 2005;62(3):247–53.
doi:10.1001/archpsyc.62.3.247
. PMID 15753237
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 20/65
.
11. ^ a b Cullen KR, Kumra S, Regan J et al.. Atypical Antipsychotics for Treatment of
Schizophrenia Spectrum Disorders
. Psychiatric Times. 2008;25(3).
12. Addington J. North American prodrome longitudinal study: a collaborative multisite
approach to prodromal schizophrenia research
. Schizophrenia Bulletin. 2007;33(3):665–72. doi:10.1093/schbul/sbl075
. PMID 17255119
.
13. Parnas J. Pre-morbid psychopathology in schizophrenia spectrum. British Journal of
Psychiatry. 1989;115:623–7. PMID 2611591
.
14. Amminger GP. Early-onset of symptoms predicts conversion to non-affective psychosis in
ultra-high risk individuals. Schizophrenia Research. 2006;84(1):67–76.
doi:10.1016/j.schres.2006.02.018
. PMID 16677803
.
15. Schneider, K (1959). Clinical Psychopathology
(5 ed.). New York: Grune & Stratton.
16. Nordgaard J, Arnfred SM, Handest P, Parnas J. The diagnostic status of first-rank
symptoms
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 21/65
. Schizophrenia Bulletin. 2008;34(1):137–54. doi:10.1093/schbul/sbm044
. PMID 17562695
.
17. Sims A. Symptoms in the mind: an introduction to descriptive psychopathology.
Philadelphia: W. B. Saunders; 2002. ISBN 0-7020-2627-1.
18. Velligan DI and Alphs LD. Negative Symptoms in Schizophrenia: The Importance of
Identification and Treatment
. Psychiatric Times. March 1, 2008;25(3).
19. Jakobsen KD. Reliability of clinical ICD-10 schizophrenia diagnoses. Nordic Journal of
Psychiatry. 2005;59(3):209–12. doi:10.1080/08039480510027698
. PMID 16195122
.
20. Pope HG. Distinguishing bipolar disorder from schizophrenia in clinical practice: guidelines
and case reports
[PDF]. Hospital and Community Psychiatry. 1983 [cited 2008-02-24];34:322–28.
21. McGlashan TH. Testing DSM-III symptom criteria for schizotypal and borderline
personality disorders. Archives of General Psychiatry. 1987 [cited 2008-07-
03];44(2):143–8. PMID 3813809
.
22. Bottas A. Comorbidity: Schizophrenia With Obsessive-Compulsive Disorder
. Psychiatric Times. April 15, 2009;26(4).
23. American Psychiatric Association DSM-5 Work Groups (2010) Proposed Revisions -
Schizophrenia and Other Psychotic Disorders
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 22/65
. Retrieved 17 February 2010.
24. Boyle, Mary. Schizophrenia: a scientific delusion?. New York: Routledge; 2002. ISBN 0-
415-22718-6.
25. Bentall, Richard P.; Read, John E; Mosher, Loren R.. Models of Madness: Psychological,
Social and Biological Approaches to Schizophrenia. Philadelphia: Brunner-Routledge;
2004. ISBN 1-58391-906-6.
26. Schizophrenia term use 'invalid'
. BBC News online (United Kingdom). 9 October 2006 [cited 16 May 2007].
27. CASL Biography
[cited 2009-02-01].[dead link] and CASL History
[cited 2009-02-01].[dead link]
28. ^ a b Tsuang MT. Toward reformulating the diagnosis of schizophrenia. American
Journal of Psychiatry. 2000;157(7):1041–50. doi:10.1176/appi.ajp.157.7.1041
. PMID 10873908
.
29. Peralta V, Cuesta MJ. A dimensional and categorical architecture for the classification of
psychotic disorders
. World Psychiatry. 2007;6(2):100–1. PMID 18235866
.
30. Verdoux H. Psychotic symptoms in non-clinical populations and the continuum of
psychosis. Schizophrenia Research. 2002;54(1–2):59–65. doi:10.1016/S0920-
9964(01)00352–8 (inactive 2009-12-08). PMID 11853979
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 23/65
.
31. Johns LC. The continuity of psychotic experiences in the general population. Clinical
Psychology Review. 2001;21(8):1125–41. doi:10.1016/S0272-7358(01)00103–9
(inactive 2010-03-22). PMID 11702510
.
32. Peters ER. Measuring delusional ideation: the 21-item Peters et al. Delusions Inventory
(PDI). Schizophrenia Bulletin. 2005;30(4):1005–22. PMID 15954204
.
33. Edgar Jones. The Phenomenology of Abnormal Belief: A Philosophical and Psychiatric
Inquiry
. Philosophy, Psychiatry and Psychology. 1999 [cited 2008-02-24];6(1):1–16.
doi:10.1353/ppp.1999.0004 (inactive 2009-12-08).
34. David AS. On the impossibility of defining delusions
. Philosophy, Psychiatry and Psychology. 1999 [cited 2008-02-24];6(1):17–20.
doi:10.1353/ppp.1999.0006 (inactive 2009-12-08).
35. S. Nassir Ghaemi. An Empirical Approach to Understanding Delusions
. Philosophy, Psychiatry and Psychology. 1999 [cited 2008-02-24];6(1):21–24.
doi:10.1353/ppp.1999.0007 (inactive 2009-12-08).
36. Andreasen NC. Schizophrenia: the fundamental questions
. Brain Res. Brain Res. Rev.. 2000;31(2–3):106–12. doi:10.1016/S0165-0173(99)00027-
2
. PMID 10719138
.
37. Andreasen NC. A unitary model of schizophrenia: Bleuler's "fragmented phrene" as
schizencephaly
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 24/65
. Archives of General Psychiatry. 1999;56(9):781–7. doi:10.1001/archpsyc.56.9.781
. PMID 12884883
.
38. ^ a b Jansson LB, Parnas J. Competing definitions of schizophrenia: what can be learned
from polydiagnostic studies?
. Schizophr Bull. 2007;33(5):1178–200. doi:10.1093/schbul/sbl065
. PMID 17158508
.
39. Green MF, Nuechterlein KH. Should schizophrenia be treated as a neurocognitive
disorder?
. Schizophr Bull. 1999;25(2):309–19. PMID 10416733
.
40. Green, Michael (2001). Schizophrenia revealed: from neurons to social interactions.
New York: W.W. Norton. ISBN 0-393-70334-7. Lay summary
.
41. Lake CR, Hurwitz N. Schizoaffective disorder merges schizophrenia and bipolar disorders
as one disease—there is no schizoaffective disorder
. Curr Opin Psychiatry. 2007;20(4):365–79. doi:10.1097/YCO.0b013e3281a305ab
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 25/65
. PMID 17551352
.
42. Malhi GS, Green M, Fagiolini A, Peselow ED, Kumari V. Schizoaffective disorder:
diagnostic issues and future recommendations. Bipolar Disorders. 2008;10(1 Pt 2):215–
30. doi:10.1111/j.1399-5618.2007.00564.x
. PMID 18199238
.
43. Craddock N, Owen MJ. The beginning of the end for the Kraepelinian dichotomy
. Br J Psychiatry. 2005;186:364–6. doi:10.1192/bjp.186.5.364
. PMID 15863738
.
44. Cooper, David A.. The Dialectics of Liberation (Pelican). London, England: Penguin Books
Ltd; 1969. ISBN 0-14-021029-6.
45. Szasz, Thomas Stephen. The myth of mental illness: foundations of a theory of personal
conduct. San Francisco: Harper & Row; 1974. ISBN 0-06-091151-4.
46. Meyer-Lindenberg A. Reduced prefrontal activity predicts exaggerated striatal
dopaminergic function in schizophrenia. Nature Neuroscience. 2002;5(3):267–71.
doi:10.1038/nn804
. PMID 11865311
.
47. Harrison PJ. Genes for schizophrenia? Recent findings and their pathophysiological
implications. The Lancet. 2003;361(9355):417–19. doi:10.1016/S0140-6736(03)12379–
3 (inactive 2009-12-08). PMID 12573388
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 26/65
.
48. Day R. Stressful life events preceding the acute onset of schizophrenia: a cross-national
study from the World Health Organization. Culture, Medicine and Psychiatry.
1987;11(2):123–205. doi:10.1007/BF00122563
. PMID 3595169
.
49. Corcoran C. The stress cascade and schizophrenia: etiology and onset. Schizophrenia
Bulletin. 2003;29(4):671–92. PMID 14989406
.
50. O'Donovan MC, Williams NM, Owen MJ. Recent advances in the genetics of schizophrenia.
Hum. Mol. Genet.. 2003;12 Spec No 2:R125–33. doi:10.1093/hmg/ddg302
. PMID 12952866
.
51. Owen MJ, Craddock N, O'Donovan MC. Schizophrenia: genes at last?. Trends Genet..
2005;21(9):518–25. doi:10.1016/j.tig.2005.06.011
. PMID 16009449
.
52. Craddock N, O'Donovan MC, Owen MJ. Genes for schizophrenia and bipolar disorder?
Implications for psychiatric nosology
. Schizophr Bull. 2006;32(1):9–16. doi:10.1093/schbul/sbj033
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 27/65
. PMID 16319375
.
53. Datta SR, McQuillin A, Rizig M, et al.. A threonine to isoleucine missense mutation in the
pericentriolar material 1 gene is strongly associated with schizophrenia. Mol. Psychiatry.
2010;15(6):615–28. doi:10.1038/mp.2008.128
. PMID 19048012
.
54. Hennah W, Thomson P, McQuillin A, et al.. DISC1 association, heterogeneity and interplay
in schizophrenia and bipolar disorder. Mol. Psychiatry. 2009;14(9):865–73.
doi:10.1038/mp.2008.22
. PMID 18317464
.
55. O'Donovan MC, Craddock NJ, Owen MJ. Genetics of psychosis; insights from views across
the genome. Hum. Genet.. 2009;126(1):3–12. doi:10.1007/s00439-009-0703-0
. PMID 19521722
.
56. Purcell SM, Wray NR, Stone JL, et al.. Common polygenic variation contributes to risk of
schizophrenia and bipolar disorder. Nature. 2009;460(7256):748–52.
doi:10.1038/nature08185
. PMID 19571811
.
57. Sanders AR, Duan J, Levinson DF, et al.. No significant association of 14 candidate genes
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 28/65
with schizophrenia in a large European ancestry sample: implications for psychiatric
genetics. Am J Psychiatry. 2008;165(4):497–506. doi:10.1176/appi.ajp.2007.07101573
. PMID 18198266
.
58. Walsh T, McClellan JM, McCarthy SE et al.. Rare structural variants disrupt multiple
genes in neurodevelopmental pathways in schizophrenia. Science. 2008;320(5875):539–
43. doi:10.1126/science.1155174
. PMID 18369103
.
59. Kirov G, Grozeva D, Norton N et al.. Support for the involvement of large CNVs in the
pathogenesis of schizophrenia
. Hum Mol Genet. 2009;18(8):1497. doi:10.1093/hmg/ddp043
. PMID 19181681
.
60. The International Schizophrenia Consortium. Rare chromosomal deletions and
duplications increase risk of schizophrenia. Nature. 11 September 2008;455(7210):237–
41. doi:10.1038/nature07239
. PMID 18668038
.
61. Crespi B, Stead P, Elliot M. Evolution in health and medicine Sackler colloquium:
Comparative genomics of autism and schizophrenia
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 29/65
. Proc. Natl. Acad. Sci. U.S.A.. 2010;107 Suppl 1:1736–41.
doi:10.1073/pnas.0906080106
. PMID 19955444
.
62. Crow TJ. The 'big bang' theory of the origin of psychosis and the faculty of language
. Schizophrenia Research. 2008;102(1–3):31–52. doi:10.1016/j.schres.2008.03.010
. PMID 18502103
.
63. Mueser KT, Jeste DV (2008). Clinical Handbook of Schizophrenia. New York: Guilford
Press. pp. 22–23. ISBN 1593856520.
64. Davies G. A systematic review and meta-analysis of Northern Hemisphere season of birth
studies in schizophrenia. Schizophrenia Bulletin. 2003;29(3):587–93. PMID 14609251
.
65. Brown AS. Prenatal infection as a risk factor for schizophrenia
. Schizophrenia Bulletin. 2006;32(2):200–2. doi:10.1093/schbul/sbj052
. PMID 16469941
.
66. ^ a b Van Os J. Does the urban environment cause psychosis?. British Journal of
Psychiatry. 2004;184(4):287–288. doi:10.1192/bjp.184.4.287
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 30/65
. PMID 15056569
.
67. van Os J, Krabbendam L, Myin-Germeys I, Delespaul P. The schizophrenia envirome
. Current Opinion in Psychiatry. 2005 [cited 2008-07-06];18(2):141–5.
doi:10.1097/00001504-200503000-00006
. PMID 16639166
.
68. Mueser KT, McGurk SR. Schizophrenia. The Lancet. 2004;363(9426):2063–72.
doi:10.1016/S0140-6736(04)16458–1 (inactive 2009-12-08). PMID 15207959
.
69. Selten JP, Cantor-Graae E, Kahn RS. Migration and schizophrenia
. Current Opinion in Psychiatry. 2007 [cited 2008-07-06];20(2):111–115.
doi:10.1097/YCO.0b013e328017f68e
. PMID 17278906
.
70. Schenkel LS. Histories of childhood maltreatment in schizophrenia: Relationships with
premorbid functioning, symptomatology, and cognitive deficits. Schizophrenia Research.
2005;76(2–3):273–286. doi:10.1016/j.schres.2005.03.003
. PMID 15949659
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 31/65
.
71. Janssen. Childhood abuse as a risk factor for psychotic experiences. Acta Psychiatrica
Scandinavica. 2004;109(1):38–45. doi:10.1046/j.0001–690X.2003.00217.x (inactive
2009-12-08). PMID 14674957
.
72. ^ a b Bentall RP. Prospects for a cognitive-developmental account of psychotic
experiences. Br J Clin Psychol. 2007;46(Pt 2):155–73. doi:10.1348/014466506X123011
. PMID 17524210
.
73. Subotnik, KL. Are Communication Deviance and Expressed Emotion Related to Family
History of Psychiatric Disorders in Schizophrenia?. Schizophrenia Bulletin.
2002;28(4):719–29. PMID 12795501
.
74. Ten-Year Recovery Outcomes for Clients With Co-Occurring Schizophrenia and
Substance Use Disorders - Drake et al. 32 (3): 464 - Schizophrenia Bulletin
75. Ferdinand RF, Sondeijker F, van der Ende J, Selten JP, Huizink A, Verhulst FC. Cannabis
use predicts future psychotic symptoms, and vice versa. Addiction. 2005;100(5):612–8.
doi:10.1111/j.1360–0443.2005.01070.x (inactive 2009-12-08). PMID 15847618
.
76. Moore THM, Zammit S, Lingford-Hughes A et al.. Cannabis use and risk of psychotic or
affective mental health outcomes: a systematic review. Lancet. 2007;370(9584):319–
328. doi:10.1016/S0140-6736(07)61162-3
. PMID 17662880
.
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 32/65
77. Degenhardt L, Hall W, Lynskey M (2001) (PDF). Comorbidity between cannabis use and
psychosis: Modelling some possible relationships.
. Technical Report No. 121.. Sydney: National Drug and Alcohol Research Centre..
Retrieved 2006-08-19.
78. Frisher M, Crome I, Martino O, Croft P. Assessing the impact of cannabis use on trends in
diagnosed schizophrenia in the United Kingdom from 1996 to 2005. Schizophr. Res..
2009;113(2-3):123–8. doi:10.1016/j.schres.2009.05.031
. PMID 19560900
.
79. http://www.nhsconfed.org/Publications/Documents/MHN_factsheet_August_2009_FI
NAL_2.pdf
Key facts and trends in mental health, National Health Service, 2009
80. Gregg L, Barrowclough C, Haddock G. Reasons for increased substance use in psychosis.
Clin Psychol Rev. 2007;27(4):494–510. doi:10.1016/j.cpr.2006.09.004
. PMID 17240501
.
81. Kuczenski R, Segal DS. Effects of methylphenidate on extracellular dopamine, serotonin,
and norepinephrine: comparison with amphetamine. J. Neurochem.. 1997;68(5):2032–7.
doi:10.1046/j.1471-4159.1997.68052032.x (inactive 2008-12-29). PMID 9109529
.
82. Mahoney JJ, Kalechstein AD, De La Garza R, Newton TF. Presence and persistence of
psychotic symptoms in cocaine- versus methamphetamine-dependent participants. The
American Journal on Addictions. 2008;17(2):83–98. doi:10.1080/10550490701861201
. PMID 18393050
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 33/65
.
83. Larson, Michael (2006-03-30). "Alcohol-Related Psychosis"
. eMedicine. WebMD. Retrieved September 27, 2006.
84. Soyka, M. Psychopathological characteristics in alcohol hallucinosis and paranoid
schizophrenia. Acta Psychiatrica Scandinavica. 1990;81(3):255–9. doi:10.1111/j.1600-
0447.1990.tb06491.x
. PMID 2343749
.
85. Gossman, William. WebMD. Delirium Tremens
; November 19, 2005 [cited October 16, 2006].
86. Broome MR, Woolley JB, Tabraham P, et al.. What causes the onset of psychosis?.
Schizophr. Res.. 2005;79(1):23–34. doi:10.1016/j.schres.2005.02.007
. PMID 16198238
.
87. Lewis R. Should cognitive deficit be a diagnostic criterion for schizophrenia?
. Journal of Psychiatry and Neuroscience. 2004;29(2):102–113. PMID 15069464
.
88. Brüne M, Abdel-Hamid M, Lehmkämper C, Sonntag C. Mental state attribution,
neurocognitive functioning, and psychopathology: what predicts poor social competence in
schizophrenia best?. Schizophr. Res.. 2007;92(1-3):151–9.
doi:10.1016/j.schres.2007.01.006
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 34/65
. PMID 17346931
.
89. Sitskoorn MM. Cognitive deficits in relatives of patients with schizophrenia: a metaanalysis.
Schizophrenia Research. 2004;71(2):285–295.
doi:10.1016/j.schres.2004.03.007
. PMID 15474899
.
90. Kurtz MM. Neurocognitive impairment across the lifespan in schizophrenia: an update.
Schizophrenia Research. 2005;74(1):15–26. doi:10.1016/j.schres.2004.07.005
. PMID 15694750
.
91. ^ a b Cohen AS. Affective reactivity of speech and emotional experience in patients with
schizophrenia. Schizophrenia Research. 2004;69(1):7–14. doi:10.1016/S0920-
9964(03)00069–0 (inactive 2009-12-08). PMID 15145465
.
92. Horan WP. Emotional responses to psychosocial stress in schizophrenia: the role of
individual differences in affective traits and coping. Schizophrenia Research. 2003;60(2–
3):271–83. doi:10.1016/S0920-9964(02)00227-X
. PMID 12591589
.
93. Barrowclough C. Self-esteem in schizophrenia: relationships between self-evaluation,
family attitudes, and symptomatology. J Abnorm Psychol. 2003;112(1):92–9.
doi:10.1037/0021–843X.112.1.92 (inactive 2009-12-08). PMID 12653417
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 35/65
.
94. Birchwood M. The power and omnipotence of voices: subordination and entrapment by
voices and significant others. Psychol Med. 2000;30(2):337–44.
doi:10.1017/S0033291799001828
. PMID 10824654
.
95. Smith B, Fowler DG, Freeman D, et al.. Emotion and psychosis: links between depression,
self-esteem, negative schematic beliefs and delusions and hallucinations. Schizophr. Res..
2006;86(1-3):181–8. doi:10.1016/j.schres.2006.06.018
. PMID 16857346
.
96. Beck, AT. A Cognitive Model of Schizophrenia. Journal of Cognitive Psychotherapy.
2004;18(3):281–88. doi:10.1891/jcop.18.3.281.65649
.
97. Bell V. Explaining delusions: a cognitive perspective. Trends in Cognitive Science.
2006;10(5):219–26. doi:10.1016/j.tics.2006.03.004
. PMID 16600666
.
98. Freeman D, Garety PA, Kuipers E, Fowler D, Bebbington PE, Dunn G. Acting on
persecutory delusions: the importance of safety seeking. Behav Res Ther. 2007;45(1):89–
99. doi:10.1016/j.brat.2006.01.014
. PMID 16530161
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 36/65
.
99. Kuipers E, Garety P, Fowler D, Freeman D, Dunn G, Bebbington P. Cognitive, emotional,
and social processes in psychosis: refining cognitive behavioral therapy for persistent
positive symptoms
. Schizophr Bull. 2006;32 Suppl 1:S24–31. doi:10.1093/schbul/sbl014
. PMID 16885206
.
100. Kircher, Tilo; Renate Thienel (2006). "Functional brain imaging of symptoms and
cognition in schizophrenia"
. The Boundaries of Consciousness. Amsterdam: Elsevier. p. 302. ISBN 0444528768.
101. Green MF. Cognitive impairment and functional outcome in schizophrenia and bipolar
disorder. Journal of Clinical Psychiatry. 2006;67(Suppl 9):3–8. PMID 16965182
.
102. Laruelle M, Abi-Dargham A, van Dyck CH, et al.. Single photon emission computerized
tomography imaging of amphetamine-induced dopamine release in drug-free
schizophrenic subjects
. Proc. Natl. Acad. Sci. U.S.A.. 1996;93(17):9235–40. doi:10.1073/pnas.93.17.9235
. PMID 8799184
.
103. Jones HM. Dopamine and antipsychotic drug action revisited. British Journal of
Psychiatry. 2002;181:271–275. doi:10.1192/bjp.181.4.271
. PMID 12356650
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 37/65
.
104. Konradi C. Molecular aspects of glutamate dysregulation: implications for schizophrenia
and its treatment. Pharmacology and Therapeutics. 2003;97(2):153–79.
doi:10.1016/S0163-7258(02)00328–5 (inactive 2009-12-08). PMID 12559388
.
105. Lahti AC. Effects of ketamine in normal and schizophrenic volunteers.
Neuropsychopharmacology. 2001;25(4):455–67. doi:10.1016/S0893-133X(01)00243–3
(inactive 2009-12-08). PMID 11557159
.
106. Coyle JT. Converging evidence of NMDA receptor hypofunction in the pathophysiology of
schizophrenia. Annals of the New York Academy of Sciences. 2003;1003:318–27.
doi:10.1196/annals.1300.020
. PMID 14684455
.
107. Tuominen HJ. Glutamatergic drugs for schizophrenia: a systematic review and metaanalysis.
Schizophrenia Research. 2005;72(2-3):225–34.
doi:10.1016/j.schres.2004.05.005
. PMID 15560967
.
108. Steen RG, Mull C, McClure R, Hamer RM, Lieberman JA. Brain volume in first-episode
schizophrenia: systematic review and meta-analysis of magnetic resonance imaging
studies
. Br J Psychiatry. 2006;188:510–8. doi:10.1192/bjp.188.6.510
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 38/65
. PMID 16738340
.
109. Lieberman JA, Bymaster FP, Meltzer HY, et al.. Antipsychotic drugs: comparison in
animal models of efficacy, neurotransmitter regulation, and neuroprotection. Pharmacol.
Rev.. 2008;60(3):358–403. doi:10.1124/pr.107.00107
. PMID 18922967
.
110. DeLisi LE. The concept of progressive brain change in schizophrenia: implications for
understanding schizophrenia
. Schizophr Bull. 2008;34(2):312–21. doi:10.1093/schbul/sbm164
. PMID 18263882
. PMC 2632405
.
111. Ellison-Wright I, Bullmore E. Meta-analysis of diffusion tensor imaging studies in
schizophrenia
. Schizophr. Res.. 2009;108(1–3):3–10. doi:10.1016/j.schres.2008.11.021
. PMID 19128945
.
112. Broyd SJ, Demanuele C, Debener S, Helps SK, James CJ, Sonuga-Barke EJS. Default-
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 39/65
mode brain dysfunction in mental disorders: a systematic review. Neurosci Biobehav Rev.
2008;33(3):279. doi:10.1016/j.neubiorev.2008.09.002
. PMID 18824195
.
113. Cannon TD, Cornblatt B, McGorry P. The empirical status of the ultra high-risk
(prodromal) research paradigm
. Schizophrenia Bulletin. 2007 [cited 2008-07-06];33(3):661–4.
doi:10.1093/schbul/sbm031
. PMID 17470445
. PMC 2526144
.
114. Drake RJ, Lewis SW. Early detection of schizophrenia
. Current Opinion in Psychiatry. 2005 [cited 2008-07-06];18(2):147–50.
doi:10.1097/00001504-200503000-00007
. PMID 16639167
.
115. Van Os J, Delespaul P. Toward a world consensus on prevention of schizophrenia.
Dialogues Clin Neurosci. 2005;7(1):53–67. PMID 16060596
.
116. Ethics and early intervention in psychosis: keeping up the pace and staying in step..
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 40/65
Schizophr Res. 2001;51(1):17–29. doi:10.1016/S0920-9964(01)00235-3
. PMID 11479062
.
117. Haroun N, Dunn L, Haroun A, Cadenhead KS. Risk and protection in prodromal
schizophrenia: ethical implications for clinical practice and future research
. Schizophrenia Bulletin. 2006 [cited 2008-07-06];32(1):166–78.
doi:10.1093/schbul/sbj007
. PMID 16207892
. PMC 2632176
.
118. Häfner H, Maurer K, Ruhrmann S, et al.. Early detection and secondary prevention of
psychosis: facts and visions. European Archives of Psychiatry and Clinical Neuroscience.
2004 [cited 2008-07-06];254(2):117–28. doi:10.1007/s00406-004-0508-z
. PMID 15146341
.
119. The positive and negative syndrome scale (PANSS) for schizophrenia.. Schizophrenia
Bulletin. 1987;13(2):261–76. PMID 3616518
.
120. Turner T.. Unlocking psychosis. British Medical Journal. 2007;334(suppl):s7.
doi:10.1136/bmj.39034.609074.94
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 41/65
. PMID 17204765
.
121. ^ a b c Bellack AS. Scientific and consumer models of recovery in schizophrenia:
concordance, contrasts, and implications
. Schizophrenia Bulletin. 2006;32(3):432–42. doi:10.1093/schbul/sbj044
. PMID 16461575
.
122. Cognitive training for supported employment: 2-3 year outcomes of a randomized
controlled trial.
. American Journal of Psychiatry. 2007;164(3):437–41. doi:10.1176/appi.ajp.164.3.437
. PMID 17329468
.
123. Outcome of schizophrenia: some transcultural observations with particular reference to
developing countries.. Eur Arch Psychiatry Clin Neurosci. 1994;244(5):227–35.
doi:10.1007/BF02190374
. PMID 7893767
.
124. National Collaborating Centre for Mental Health. Gaskell and the British Psychological
Society. Schizophrenia: Full national clinical guideline on core interventions in primary
and secondary care
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 42/65
[PDF]; 2009-03-25 [cited 2009-11-25].
125. Murphy BP, Chung YC, Park TW, McGorry PD. Pharmacological treatment of primary
negative symptoms in schizophrenia: a systematic review
. Schizophrenia Research. 2006;88(1–3):5–25. doi:10.1016/j.schres.2006.07.002
. PMID 16930948
.
126. Gray JA, Roth BL. The pipeline and future of drug development in schizophrenia.
Molecular Psychiatry. 2007;12(10):904–22. doi:10.1038/sj.mp.4002062
. PMID 17667958
.
127. Jarskog LF, Miyamoto S, Lieberman JA. Schizophrenia: new pathological insights and
therapies
. Annu. Rev. Med.. 2007;58:49–61. doi:10.1146/annurev.med.58.060904.084114
. PMID 16903799
.
128. Tandon R, Keshavan MS, Nasrallah HA. Schizophrenia, "Just the Facts": what we know in
2008 part 1: overview
. Schizophrenia Research. 2008;100(1-3):4–19. doi:10.1016/j.schres.2008.01.022
. PMID 18291627
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 43/65
.
129. Lieberman JA, Stroup TS, McEvoy JP, et al.. Effectiveness of antipsychotic drugs in
patients with chronic schizophrenia
. New England Journal of Medicine. 2005 [cited 2008-07-04];353(12):1209–23.
doi:10.1056/NEJMoa051688
. PMID 16172203
.
130. "Clinical Antipsychotic Trials of Intervention Effectiveness (CATIE)"
. National Institute of Mental Health. Retrieved June 16, 2010.
131. Swartz MS, Stroup TS et al.. What CATIE Found: Results From the Schizophrenia Trial
. Psychiatric Services. 2008;59(5):500–06. doi:10.1176/appi.ps.59.5.500
. PMID 18451005
.
132. Leucht S, Wahlbeck K, Hamann J, Kissling W. New generation antipsychotics versus lowpotency
conventional antipsychotics: a systematic review and meta-analysis
. Lancet. 2003 [cited 2008-07-04];361(9369):1581–89. doi:10.1016/S0140-
6736(03)13306-5
. PMID 12747876
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 44/65
.
133. Dickson RA, Dalby JT, Williams R, Edwards AL. Risperidone-induced prolactin elevations
in premenopausal women with schizophrenia. American Journal of Psychiatry.
1995;152(7):1102–03. PMID 7540803
.
134. Ananth J, Parameswaran S, Gunatilake S, Burgoyne K, Sidhom T. Neuroleptic malignant
syndrome and atypical antipsychotic drugs
. Journal of Clinical Psychiatry. 2004 [cited 2008-07-04];65(4):464–70.
doi:10.4088/JCP.v65n0403
. PMID 15119907
.
135. Meltzer HY. Treatment-resistant schizophrenia—the role of clozapine. Current Medical
Research and Opinion. 1997;14(1):1–20. doi:10.1185/03007999709113338
. PMID 9524789
.
136. Wahlbeck K, Cheine MV, Essali A. Clozapine versus typical neuroleptic medication for
schizophrenia. The Cochrane Database of Systematic Reviews. 2007;(2):CD000059.
doi:10.1002/14651858.CD000059
. PMID 10796289
.
137. Haas SJ, Hill R, Krum H. Clozapine-associated myocarditis: a review of 116 cases of
suspected myocarditis associated with the use of clozapine in Australia during 1993–2003.
Drug Safety. 2007;30(1):47–57. doi:10.2165/00002018-200730010-00005
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 45/65
. PMID 17194170
.
138. Moran, M. Psychosocial Treatment Often Missing From Schizophrenia Regimens
. Psychiatric News. 18 November 2005 [cited 17 May 2007];40(22):24.
139. Sensky T, Turkington D, Kingdon D, Scott JL, Scott J, Siddle R, O'Carroll M, Barnes TR. A
randomized controlled trial of cognitive-behavioral therapy for persistent symptoms in
schizophrenia resistant to medication. Archives of General Psychiatry. 2000;57(2):165–
72. doi:10.1001/archpsyc.57.2.165
. PMID 10665619
.
140. Kuipers E, Garety P, Fowler D, Dunn G, Bebbington P, Freeman D, Hadley C. London-
East Anglia randomised controlled trial of cognitive-behavioural therapy for psychosis. I:
effects of the treatment phase. Br J Psychiatry. 1997;171:319–27.
doi:10.1192/bjp.171.4.319
. PMID 9373419
.
141. Lewis S, Tarrier N, Haddock G, Bentall R, Kinderman P, Kingdon D, Siddle R, Drake R,
Everitt J, Leadley K, Benn A, Grazebrook K, Haley C, Akhtar S, Davies L, Palmer S,
Faragher B, Dunn G. Randomised controlled trial of cognitive-behavioural therapy in early
schizophrenia: acute-phase outcomes. Br J Psychiatry Suppl. 2002;43:s91–7. PMID
12271807
.
142. Cormac I, Jones C, Campbell C. Cognitive behaviour therapy for schizophrenia. Cochrane
Database of systematic reviews. 2002 [cited 2008-07-03];(1):CD000524.
doi:10.1002/14651858.CD000524
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 46/65
. PMID 11869579
.
143. Wykes T, Steel C, Everitt B, Tarrier N. Cognitive behavior therapy for schizophrenia:
effect sizes, clinical models, and methodological rigor
. Schizophr Bull. 2008;34(3):523–37. doi:10.1093/schbul/sbm114
. PMID 17962231
.
144. Zimmermann G, Favrod J, Trieu VH, Pomini V. The effect of cognitive behavioral
treatment on the positive symptoms of schizophrenia spectrum disorders: a metaanalysis
. Schizophrenia Research. 2005 [cited 2008-07-03];77(1):1–9.
doi:10.1016/j.schres.2005.02.018
. PMID 16005380
.
145. Lynch D, Laws KR, McKenna PJ. Cognitive behavioural therapy for major psychiatric
disorder: does it really work? A meta-analytical review of well-controlled trials. Psychol
Med. 2010;40(1):9–24. doi:10.1017/S003329170900590X
. PMID 19476688
.
146. Wykes T, Brammer M, Mellers J, et al.. Effects on the brain of a psychological treatment:
cognitive remediation therapy: functional magnetic resonance imaging in schizophrenia
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 47/65
. British Journal of Psychiatry. 2002 [cited 2008-07-03];181:144–52.
doi:10.1192/bjp.181.2.144
. PMID 12151286
.
147. Medalia A. Cognitive Remediation for Psychiatric Patients: Improving Functional
Outcomes for Patients With Schizophrenia
. Psychiatric Times. 2009;26(3).
148. Hogarty GE, Flesher S, Ulrich R, et al.. Cognitive enhancement therapy for schizophrenia:
effects of a 2-year randomized trial on cognition and behavior
. Archives of General Psychiatry. 2004 [cited 2008-07-03];61(9):866–76.
doi:10.1001/archpsyc.61.9.866
. PMID 15351765
.
149. McFarlane WR, Dixon L, Lukens E, Lucksted A. Family psychoeducation and
schizophrenia: a review of the literature. J Marital Fam Ther. 2003;29(2):223–45.
doi:10.1111/j.1752–0606.2003.tb01202.x (inactive 2009-12-08). PMID 12728780
.
150. Glynn SM, Cohen AN, Niv N. New challenges in family interventions for schizophrenia
. Expert Review of Neurotherapeutics. 2007 [cited 2008-07-03];7(1):33–43.
doi:10.1586/14737175.7.1.33
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 48/65
. PMID 17187495
.
151. Family intervention for schizophrenia.
. Cochrane Database Syst Rev. 2006;(4):CD000088.
doi:10.1002/14651858.CD000088.pub2
. PMID 17054127
.
152. Jones S, Hayward P. Coping with Schizophrenia: A Guide for Patients, Families and
Caregivers. Oxford, England: Oneworld Pub.; 2004. ISBN 1-85168-344-5.
153. Torrey EF. Surviving Schizophrenia: A Manual for Families, Consumers, and Providers.
5th ed. HarperCollins; 2006. ISBN 0-06-084259-8.
154. Kopelowicz A, Liberman RP, Zarate R. Recent advances in social skills training for
schizophrenia
. Schizophrenia Bulletin. 2006 [cited 2008-07-03];32 Suppl 1:S12–23.
doi:10.1093/schbul/sbl023
. PMID 16885207
. PMC 2632540
.
155. American Psychiatric Association (February 2004). "Practice Guideline for the Treatment
of Patients With Schizophrenia. Second Edition"
. USA: National Guideline Clearinghouse.
156. Talwar N, Crawford MJ, Maratos A, Nur U, McDermott O, Procter S. Music therapy for
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 49/65
in-patients with schizophrenia: exploratory randomised controlled trial
. The British Journal of Psychiatry. 2006 [cited 2008-07-03];189:405–9.
doi:10.1192/bjp.bp.105.015073
. PMID 17077429
.
157. Art therapy for schizophrenia or schizophrenia-like illnesses.
. Cochrane Database Syst Rev. 2005;(4):CD003728.
doi:10.1002/14651858.CD003728.pub2
. PMID 16235338
.
158. Drama therapy for schizophrenia or schizophrenia-like illnesses.
. Cochrane Database Syst Rev. 2007;(1):CD005378.
doi:10.1002/14651858.CD005378.pub2
. PMID 17253555
.
159. Mosher LR. Soteria and other alternatives to acute psychiatric hospitalization: a personal
and professional review
. Journal of Nervous and Mental Disease. 1999 [cited 2008-07-03];187(3):142–9.
doi:10.1097/00005053-199903000-00003
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 50/65
. PMID 10086470
.
160. Calton T, Ferriter M, Huband N, Spandler H. A systematic review of the Soteria paradigm
for the treatment of people diagnosed with schizophrenia
. Schizophrenia Bulletin. 2008 [cited 2008-07-03];34(1):181–92.
doi:10.1093/schbul/sbm047
. PMID 17573357
. PMC 2632384
.
161. Greenhalgh J, Knight C, Hind D, Beverley C, Walters S. Clinical and cost-effectiveness of
electroconvulsive therapy for depressive illness, schizophrenia, catatonia and mania:
systematic reviews and economic modelling studies. Health Technol Assess.. 2005 [cited
2007-06-17];9(9):1–156. PMID 15774232
.
162. "The clinical effectiveness and cost effectiveness of electroconvulsive Therapy (ECT) for
depressive illness, schizophrenia, catatonia and mania."
. National Institute for Health and Clinical Excellence. April 2003. Retrieved 2007-06-17.
163. Mashour GA, Walker EE, Martuza RL. Psychosurgery: past, present, and future
. Brain Res. Brain Res. Rev.. 2005 [cited 2008-07-04];48(3):409–19.
doi:10.1016/j.brainresrev.2004.09.002
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 51/65
. PMID 15914249
.
164. Goering P, Durbin J, Sheldon CT, Ochocka J, Nelson G, Krupa T. Who uses consumer-run
self-help organizations?
. American Journal of Orthopsychiatry. 2006 [cited 2008-07-04];76(3):367–73.
doi:10.1037/0002-9432.76.3.367
. PMID 16981815
.
165. Gorczynski, P.; Faulkner, G.; Faulkner, G. (2010). "Exercise therapy for schizophrenia".
Cochrane database of systematic reviews (Online) 5: CD004412.
doi:10.1002/14651858.CD004412.pub2
. PMID 20464730
. edit
166. Harrison G, Hopper K, Craig T, et al.. Recovery from psychotic illness: a 15- and 25-year
international follow-up study
. British Journal of Psychiatry. 2001 [cited 2008-07-04];178:506–17.
doi:10.1192/bjp.178.6.506
. PMID 11388966
.
167. ^ a b Jobe TH, Harrow M. Long-term outcome of patients with schizophrenia: a review
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 52/65
[PDF]. Canadian Journal of Psychiatry. 2005 [cited 2008-07-05];50(14):892–900.
PMID 16494258
.
168. Robinson DG, Woerner MG, McMeniman M, Mendelowitz A, Bilder RM. Symptomatic and
functional recovery from a first episode of schizophrenia or schizoaffective disorder
. American Journal of Psychiatry. 2004 [cited 2008-07-04];161(3):473–9.
doi:10.1176/appi.ajp.161.3.473
. PMID 14992973
.
169. Harvey CA, Jeffreys SE, McNaught AS, Blizard RA, King MB. The Camden Schizophrenia
Surveys III: Five-Year Outcome of a Sample of Individuals From a Prevalence Survey
and the Importance of Social Relationships
. International Journal of Social Psychiatry. 2007 [cited 2008-07-04];53(4):340–356.
doi:10.1177/0020764006074529
. PMID 17703650
.
170. Hopper K, Wanderling J. Revisiting the developed versus developing country distinction in
course and outcome in schizophrenia: results from ISoS, the WHO collaborative followup
project. International Study of Schizophrenia
. Schizophrenia Bulletin. 1 January 2000 [cited 2008-07-04];26(4):835–46. PMID
11087016
.
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 53/65
171. Andreasen NC, Carpenter WT, Kane JM, Lasser RA, Marder SR, Weinberger DR.
Remission in schizophrenia: proposed criteria and rationale for consensus
. The American Journal of Psychiatry. 2005 [cited 2008-07-07];162(3):441–9.
doi:10.1176/appi.ajp.162.3.441
. PMID 15741458
.
172. Liberman RP, Kopelowicz A. Recovery From Schizophrenia: A Concept in Search of
Research
. Psychiatric Services. 2005 [cited 2008-07-07];56(6):735–742.
doi:10.1176/appi.ps.56.6.735
. PMID 15939952
.
173. Davidson L, Schmutte T, Dinzeo T, Andres-Hyman R. Remission and recovery in
schizophrenia: practitioner and patient perspectives
. Schizophrenia Bulletin. 2008 [cited 2008-07-07];34(1):5–8.
doi:10.1093/schbul/sbm122
. PMID 17984297
. PMC 2632379
.
174. Davidson L, McGlashan TH. The varied outcomes of schizophrenia. Canadian Journal of
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 54/65
Psychiatry. 1997;42(1):34–43. PMID 9040921
.
175. Lieberman JA, Koreen AR, Chakos M, et al.. Factors influencing treatment response and
outcome of first-episode schizophrenia: implications for understanding the
pathophysiology of schizophrenia. Journal of Clinical Psychiatry. 1996;57 Suppl 9:5–9.
PMID 8823344
.
176. Bebbington P, Kuipers L. The predictive utility of expressed emotion in schizophrenia: an
aggregate analysis. Psychological Medicine. 1994;24(3):707–18.
doi:10.1017/S0033291700027860
. PMID 7991753
.
177. Hannerz H, Borgå P, Borritz M. Life expectancies for individuals with psychiatric
diagnoses. Public Health. 2001;115(5):328–37. doi:10.1038/sj.ph.1900785
. PMID 11593442
.
178. Evins AE. Nicotine Dependence in Schizophrenia: Prevalence, Mechanisms, and
Implications for Treatment
. Psychiatric Times. March 1, 2008;25(3).
179. Palmer BA, Pankratz VS, Bostwick JM. The lifetime risk of suicide in schizophrenia: a
reexamination. Archives of General Psychiatry. 2005;62(3):247–53.
doi:10.1001/archpsyc.62.3.247
. PMID 15753237
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 55/65
.
180. Radomsky ED, Haas GL, Mann JJ, Sweeney JA. Suicidal behavior in patients with
schizophrenia and other psychotic disorders
. American Journal of Psychiatry. 1 October 1999 [cited 2008-07-04];156(10):1590–5.
PMID 10518171
.
181. Caldwell CB, Gottesman II. Schizophrenics kill themselves too: a review of risk factors for
suicide. Schizophr Bull. 1990;16(4):571–89. PMID 2077636
.
182. Dalby JT, Williams RJ. Depression in schizophrenics. New York: Plenum Press; 1989.
ISBN 0-306-43240-4.
183. Violence and schizophrenia:
Walsh E, Buchanan A, Fahy T. Violence and schizophrenia: examining the evidence
. British Journal of Psychiatry. 2002 [cited 2008-07-04];180:490–5.
doi:10.1192/bjp.180.6.490
. PMID 12042226
.
Stuart H. Violence and mental illness: an overview
. World Psychiatry. 2003;2(2):121–24. PMID 16946914
.
Steadman HJ, Mulvey EP, Monahan J, et al.. Violence by people discharged from
acute psychiatric inpatient facilities and by others in the same neighborhoods
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 56/65
. Archives of General Psychiatry. 1998 [cited 2008-07-04];55(5):393–401.
doi:10.1001/archpsyc.55.5.393
. PMID 9596041
.
Swanson JW, Swartz MS, Van Dorn RA, et al.. A national study of violent behavior in
persons with schizophrenia
. Archives of General Psychiatry. 2006 [cited 2008-07-04];63(5):490–9.
doi:10.1001/archpsyc.63.5.490
. PMID 16651506
.
Swanson JW, Holzer CE, Ganju VK, Jono RT. Violence and psychiatric disorder in
the community: evidence from the Epidemiologic Catchment Area surveys
. Hospital and Community Psychiatry. 1990 [cited 2008-07-04];41(7):761–70.
PMID 2142118
.
184. ^ a b Mullen PE. Schizophrenia and violence: from correlations to preventive strategies
. Advances in Psychiatric Treatment. 2006 [cited 2008-07-04];12:239–248.
doi:10.1192/apt.12.4.239
.
185. Simpson AI, McKenna B, Moskowitz A, Skipworth J, Barry-Walsh J. Homicide and mental
illness in New Zealand, 1970–2000
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 57/65
. British Journal of Psychiatry. 2004 [cited 2008-07-04];185:394–8.
doi:10.1192/bjp.185.5.394
. PMID 15516547
.
186. Fazel S, Grann M. Psychiatric morbidity among homicide offenders: a Swedish population
study
. American Journal of Psychiatry. 2004 [cited 2008-07-04];161(11):2129–31.
doi:10.1176/appi.ajp.161.11.2129
. PMID 15514419
.
187. Brekke JS, Prindle C, Bae SW, Long JD. Risks for individuals with schizophrenia who are
living in the community
. Psychiatric Services. 2001 [cited 2008-07-04];52(10):1358–66.
doi:10.1176/appi.ps.52.10.1358
. PMID 11585953
.
188. Fitzgerald PB, de Castella AR, Filia KM, Filia SL, Benitez J, Kulkarni J. Victimization of
patients with schizophrenia and related disorders. The Australian and New Zealand
Journal of Psychiatry. 2005;39(3):169–74. doi:10.1111/j.1440-1614.2005.01539.x
. PMID 15701066
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 58/65
.
189. Walsh E, Gilvarry C, Samele C, et al.. Predicting violence in schizophrenia: a prospective
study
. Schizophrenia Research. 2004 [cited 2008-07-04];67(2–3):247–52.
doi:10.1016/S0920-9964(03)00091-4
. PMID 14984884
.
190. Solomon PL, Cavanaugh MM, Gelles RJ. Family violence among adults with severe mental
illness: a neglected area of research
. Trauma Violence Abuse. 2005 [cited 2008-07-04];6(1):40–54.
doi:10.1177/1524838004272464
. PMID 15574672
.{subscription required)
191. Chou KR, Lu RB, Chang M. Assaultive behavior by psychiatric in-patients and its related
factors. J Nurs Res. 2001;9(5):139–51. PMID 11779087
.
192. Lögdberg B, Nilsson LL, Levander MT, Levander S. Schizophrenia, neighbourhood, and
crime. Acta Psychiatrica Scandinavica. 2004;110(2):92–7. doi:10.1111/j.1600-
0047.2004.00322.x
. PMID 15233709
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 59/65
.
193. Kumra S. Childhood-onset schizophrenia: research update. Canadian Journal of
Psychiatry. 2001;46(10):923–30. PMID 11816313
.
194. Hassett, Anne, et al. (eds) (2005). Psychosis in the Elderly
. London: Taylor and Francis.. p. 6. ISBN 1841843946.
195. Jablensky A. Schizophrenia: manifestations, incidence and course in different cultures. A
World Health Organization ten-country study. Psychological Medicine Monograph
Supplement. 1992;20:1–97. doi:10.1017/S0264180100000904
. PMID 1565705
.
196. Kirkbride JB, Fearon P, Morgan C, et al.. Heterogeneity in incidence rates of schizophrenia
and other psychotic syndromes: findings from the 3-center AeSOP study. Archives of
General Psychiatry. 2006;63(3):250–8. doi:10.1001/archpsyc.63.3.250
. PMID 16520429
.
197. Kirkbride JB. Neighbourhood variation in the incidence of psychotic disorders in Southeast
London. Social Psychiatry and Psychiatric Epidemiology. 2007;42(6):438–45.
doi:10.1007/s00127-007-0193-0
. PMID 17473901
.
198. Ustun TB. Multiple-informant ranking of the disabling effects of different health
conditions in 14 countries. The Lancet. 1999;354(9173):111–15. doi:10.1016/S0140-
6736(98)07507-2
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 60/65
. PMID 10408486
.
199. Heinrichs RW. Historical origins of schizophrenia: two early madmen and their illness.
Journal of the History of the Behavioral Sciences. 2003;39(4):349–63.
doi:10.1002/jhbs.10152
. PMID 14601041
.
200. Kraepelin E, Diefendorf AR. Text book of psychiatry. 7 ed. London: Macmillan; 1907.
201. Hansen RA, Atchison B. Conditions in occupational therapy: effect on occupational
performance. Hagerstown, MD: Lippincott Williams & Wilkins; 2000. ISBN 0-683-
30417-8.
202. Kuhn R;. Eugen Bleuler's concepts of psychopathology. History of Psychiatry.
2004;15(3):361–6. doi:10.1177/0957154X04044603
. PMID 15386868
.
203. Stotz-Ingenlath G. Epistemological aspects of Eugen Bleuler's conception of schizophrenia
in 1911
[PDF]. Medicine, Health Care and Philosophy. 2000 [cited 2008-07-03];3(2):153–9.
doi:10.1023/A:1009919309015
. PMID 11079343
.
204. Wing JK. International comparisons in the study of the functional psychoses. British
Medical Bulletin. 1971;27(1):77–81. PMID 4926366
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 61/65
.
205. Rosenhan D. On being sane in insane places. Science. 1973;179(70):250–8.
doi:10.1126/science.179.4070.250
. PMID 4683124
.
206. Wilson M. DSM-III and the transformation of American psychiatry: a history
. American Journal of Psychiatry. 1993 [cited 2008-07-03];150(3):399–410. PMID
8434655
.{subscription required}
207. Porter, Roy; Berrios, G. E. (1995). A history of clinical psychiatry: the origin and history
of psychiatric disorders. London: Athlone Press. ISBN 0-485-24211-7.
208. Maj, Mario and Sartorius N.. Schizophrenia. Chichester: Wiley; 15 September 1999. ISBN
978-0-471-99906-5. p. 292.
209. Pescosolido BA, Monahan J, Link BG, Stueve A, Kikuzawa S. The public's view of the
competence, dangerousness, and need for legal coercion of persons with mental health
problems
. American Journal of Public Health. 1999 [cited 2008-07-03];89(9):1339–45.
doi:10.2105/AJPH.89.9.1339
. PMID 10474550
. PMC 1508769
.
210. Phelan JC, Link BG, Stueve A, Pescosolido BA. Public Conceptions of Mental Illness in
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 62/65
1950 and 1996: What Is Mental Illness and Is It to be Feared?
. Journal of Health and Social Behavior. 2000;41(2):188–207. doi:10.2307/2676305
.
211. Kim Y, Berrios GE. Impact of the term schizophrenia on the culture of ideograph: the
Japanese experience. Schizophr Bull. 2001;27(2):181–5. PMID 11354585
.
212. Sato M. Renaming schizophrenia: a Japanese perspective
. World Psychiatry. 2004;5(1):53–55. PMID 16757998
.
213. Deveson A (1991). Tell Me I'm Here. Penguin. ISBN 0-14-027257-7.
Further reading
Bentall, Richard. Madness explained: psychosis and human nature. London: Allen Lane;
2003. ISBN 0-7139-9249-2.
Dalby, J. Thomas. Mental disease in history: a selection of translated readings. Bern:
Peter Lang; 1996. ISBN 0-8204-3056-0.
Fallon, James H.. The Neuroanatomy of Schizophrenia: Circuitry and Neurotransmitter
Systems. Clinical Neuroscience Research. 2003 [cited 2008-07-07];3:77–107.
doi:10.1016/S1566-2772(03)00022-7
.
Fleck, Stephen; Theodore Lidz; and Alice Cornelison. Schizophrenia and the family. New
York: International Universities Press; 1985. ISBN 0-8236-6001-X.
Keen TM. Schizophrenia: orthodoxy and heresies. A review of alternative possibilities.
Journal of Psychiatric and Mental Health Nursing. 1999;6(6):415–24.
doi:10.1046/j.1365-2850.1999.00237.x
. PMID 10818864
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 63/65
.
Laing, Ronald D.. The divided self: an existential study in sanity and madness. New York:
Penguin Books; 1990. ISBN 0-14-013537-5.
Lenzenweger, M.F. (2010). Schizotypy and schizophrenia: The view from experimental
psychopathology. New York: Guilford Press. ISBN 978-1-60623-865-3
Noll, Richard. The Encyclopedia of Schizophrenia And Other Psychotic Disorders (Facts
on File Library of Health and Living). New York: Facts on File; 2006. ISBN 0-8160-
6405-9.
Roazen, Paul nd Victor Tausk. Sexuality, war, and schizophrenia: collected
psychoanalytic papers. New Brunswick, N.J., U.S.A: Transaction Publishers; 1991. ISBN
0-88738-365-3. (On the Origin of the 'Influencing Machine' in Schizophrenia.)
Shaner A, Miller G, Mintz J. Schizophrenia as one extreme of a sexually selected fitness
indicator
[PDF]. Schizophr. Res.. 2004 [cited 2008-07-07];70(1):101–9.
doi:10.1016/j.schres.2003.09.014
. PMID 15246469
.
Szasz, Thomas Stephen (1976). Schizophrenia: the sacred symbol of psychiatry. New
York: Basic Books. ISBN 0-465-07222-4.
Walker Elaine, et al. Schizophrenia: Etiology and Course
. Annual Review of Psychology. 2004;55:401–30.
doi:10.1146/annurev.psych.55.090902.141950
. PMID 14744221
.
External links
Schizophrenia
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 64/65
at the Open Directory Project
NPR: the sight and sounds of schizophrenia
The current World Health Organisation definition of Schizophrenia
Symptoms in Schizophrenia
Film made in 1940 showing some of the symptoms of Schizophrenia.
en.wikipedia.org
http://en.wikipedia.org/wiki/Schizophrenia
http://goo.gl/ffgS
13.9.2010 г. Schizophrenia - Wikipedia, the free enc…
en.wikipedia.org/wiki/Schizophrenia 65/65